When can I run again???
One of the first questions I had postpartum was when can I run again??
I had a long and hard recovery my first time around. I had been prepping for the baby so much that I neglected to think about what my body would go through and how I would recover.
In my defense, I feel like NOBODY warned me or spoke to me about postpartum recovery!
My pregnancy and delivery were fairly normal and I can’t complain too much.

I vividly remember sitting in my hospital bed waiting for my legs to un-numb and thinking, oh crap. This is going to hurt tomorrow!
I ended up with a 2nd degree tear. Second-degree tears involve the skin and muscle of the perineum and might extend deep into the vagina. It normally requires stitches.
It took forever to heal. At my 6 week check up my doctor confirmed that it was not healed. She said that some bodies just take longer to heal. 🤷🏼♀️
I was given permission to do anything besides sex due to the tear issue. She agreed that it didn’t look quite right yet. 🙈 She gave me some estrogen cream to spead up the healing which also temporarily brought back my period. (Thank goodness it disappeared again and didn’t come back until 11 month postpartum!)
Anyway, my body was nowhere near ready to run or do anything high intensity. Which I was missing and craving!
I also felt so much heaviness and pressure in my vagina.
It was depressing.
It also didn’t help that I was comparing myself to other mothers and their pregnancy/postpartum journey. So many were running even before their 6 week check up and seemed fine and happy!
I walked a lot but any time I tried to run, I felt like I was a baby just learning to walk.
Everything felt SO weird and different.
I didn’t know what was wrong, how to fix it, etc. I ran 5 miles the day before giving birth, so I thought I’d be ready to run pretty easily postpartum.
I kept walking and worked on regaining my strength. I also did some research on the pelvic floor and began giving some focus to my core and pelvic floor.

Eventually my tear healed and the pressure and heavy feeling went away.
I did a bunch of races, including my first full Ironman before getting pregnant with baby #2.
My recovery went a lot smoother this time and I felt more equipped to handle recovery. My expectations were also set more realistically.
Pregnancy #3 and Postpartum #3 was by far the smoothest!
Since that first postpartum experience, I’ve done a handful of 5ks, 10ks, 1/2 marathons, full marathons, triathlons, 1/2 Ironmans, and 1 Full Ironman!
I don’t say this to brag, but to give encouragement.
You CAN return to running and be even stronger than you were before! It’s possible with time, the right tools and guidance.








SO, let’s get into it!!!
But first. Disclaimer: I am NOT a doctor. I’m a personal trainer, a runner, triathlete, and someone who has gone through the postpartum experience 3 times. This article is not meant to diagnose or prescribe or advise you in your situation. It is informational and hopefully something that can give you guidance and awareness as you return to run postpartum. Every person, birth, and situation is different. Always seek help from your health provider to get specific guidance for you. If you have any questions about this article or online coaching, fill out the form below. ¨̮
In this article, I’m going to discuss the following:
- Postpartum Rest and Recovery
- Why is it important to give your body time to recover?
- How long do I have to wait?
- Postpartum Deep Core
- Pelvic Floor
- Diastasis Recti
- Diaphragmatic Breathing
- Transverse Abdominis
- Deep Core Exercises
- Assessments: is your body ready to run?
- Load and Impact Assessment
- Strength Assessment
- Running Form
- Preparing to Run
- Walking
- Strength Training
- Other Things to Consider
- Posture
- Sleep
- Feet
- Nutrition
- Breastfeeding
- Feet
- Conclusion
1. Postpartum Rest and Recovery
Why is it important to give your body time to recover?
First of all, you just carried a baby for 9-10 months, gave birth, and are in charge of a tiny human with a lot of demands and needs!
Give yourself grace.
And time.
You’re tired, hormonal, and are going through a major life change. Plus, you’re body just went through a medical procedure.
You wouldn’t expect someone who just had their appendix removed or who had knee surgery to hurry and “bounce back”.
You would want them to rest and fully recover.
Avoid comparing your postpartum journey to others. Unfollow people or get off social media if you need to. This is something that I’ve had to do from time to time.
I can’t stress enough that everyone is different!
Even if this isn’t your first postpartum experience, each pregnancy and birth can vary. My first postpartum experience was drastically different from my third.
How long do I have to wait?
So, with all of that said, everyone is different. The time frame is variable depending on your pregnancy, birth, recovery, etc. etc.
However, MOST physical therapists and doctors who have researched and conducted studies, recommend waiting 3-6 months as a guideline before you resume running.
I remember reading that and I was like, nah. That’s not for me. I’m fit and athletic. I can do it sooner. Lemme sign up for a marathon. 😜 ….fast forward 6 months when I cancelled the marathon because I was not ready!
But, I get it. Runners gotta run. 🏃🏼♀️
However, you NEED to be patient if you want to avoid injury and come back stronger.
If anyone talks about bouncing back or getting your body back, just punch them in the face. 😜
Your body and tissues need to heal in order to do something so high impact and dynamic as running.
It can take 4-6 months for your tissues to fully heal.
A 2019 study by UK physiotherapist Tom Goom and colleagues Grainne Donnelly, and Emma Brockwell, suggest women wait 3-6 months before resuming running. They said,
“The levator hiatus (pelvis) widens during pregnancy and increases significantly during vaginal birth. Recovery time for the tissues is understood to be between 4-6 months, well beyond the traditional concept of full recovery by the 6-week postnatal check….
If we consider cesarean section deliveries, we understand that abdominal fascia has only regained just over 50% of original tensile strength by 6-weeks post abdominal surgery and 73%-93% of original tensile strength by 6-7 months.”
Return to Running Postnatal–guidelines for medical, health, and fitness professionals. Tom Groom, Grainne Donnelly and Emma Brockwell.
The timeline may vary from person to person. Some might need to wait longer, some might feel comfortable resuming earlier.
If you are unsure, find a good pelvic floor PT who specializes in this stuff.
It’s important to become super aware of how your body is feeling. Listen to your body. Don’t push through pain. (speaking from experience!) 🙋🏼♀️
Focus on what you can do and remember, this is temporary.
You can come back stronger and faster than ever if you put in the time and work to recover.
2. Postpartum Deep Core
Pelvic Floor
First off, definitely go see a pelvic floor therapist postpartum. They can assess your pelvic floor and core strength.
I was expecting this kind of treatment to come from my OB, but the truth is, it won’t.
They don’t have the time or knowledge to do this unfortunately. Hopefully someday this can be part of the whole giving birth package!
Okay, so what is the pelvic floor?
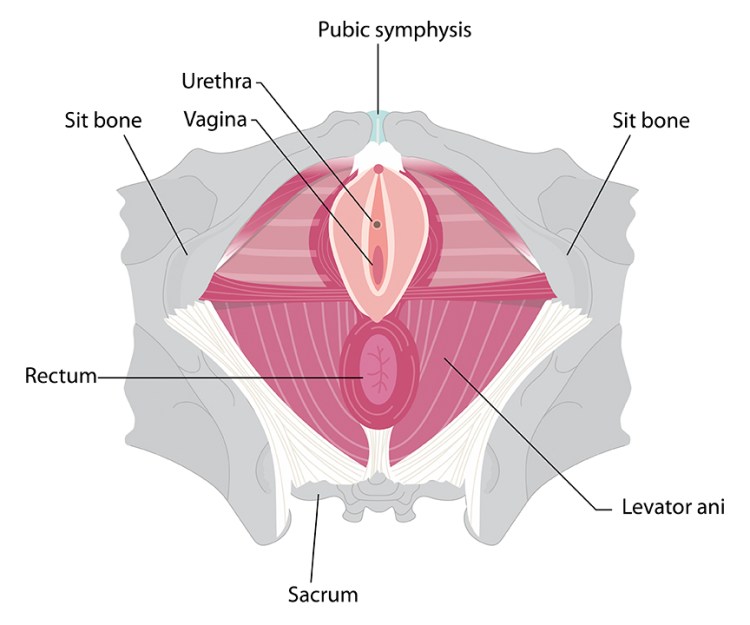
In women, the pelvic floor is a group of muscles and ligaments that support the bladder, uterus, and bowel. It’s kind of like a sling, holding everything up.

You can also think of it like a diamond. One point of the diamond is the pubic symphysis (pubic bone) and the opposite end is the Coccyx (end of the tailbone). You have your sit bones on either side.
Even if you didn’t have a vaginal birth, you can still have issues with your pelvic floor due to pregnancy.
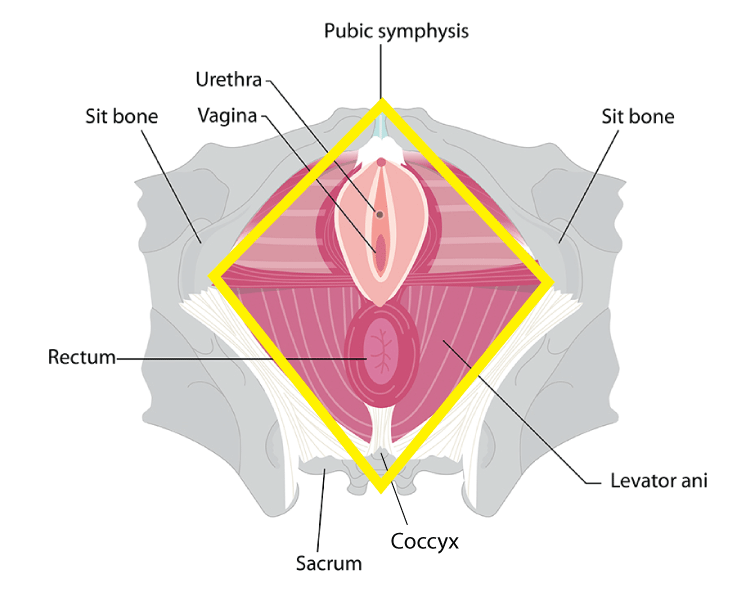
When you contract your pelvic floor muscles, your internal organs are lifted and the entrance to your anus, vagina, and urethra tighten.
This is different from a kegel. A kegal can open/close the urethra, vagina, anus, but it does not lift the pelvic floor.
One way to locate your pelvic floor is to pretend you’re peeing and the pretend to stop your stream of urine. It is not recommended to actually do this as it can lead to a UTI.
I’ve personally struggled with both a weak and tight pelvic floor.
If you are type A, and find that you clench your jaw, squeeze your butt cheeks, are unable to relax, etc. this might be you too! 🙋🏼♀️ I’ve had to learn to RELAX my pelvic floor.
This is also super important for delivering a baby vaginally. As you push, you need to relax and make more space for that little baby to come through.
Some women have a tight pelvic floor. Some women have a weak pelvic floor. And some can have a combination of both!
The tricky thing is, a lot of the symptoms of these pelvic floor dysfunctions crossover.
That is why it’s so important to get checked out by a PT. They can can do an internal exam so you can know what exercises would be most helpful.
Signs of a tight pelvic floor:
- Painful sex
- Leaking urine
- Difficulty starting to pee
- Dribbling after you pee or having to pee again right after going
- SI joint pain, tailbone, and/or hip pain
- Shallow breathing, difficulty getting a full breath in
- Constipation
Signs of a weak pelvic floor:
- Difficulty engaging your pelvic floor
- When you try to engage/contract your pelvic floor, you clench your butt, inner thighs and abs instead
- Leaking urine
- Unable to hold in gas
- Decreased sensation during sex
So why is the pelvic floor important for running?
Running is HIGH impact.
When you run, the impact is about 2 times your bodyweight! That’s a lot! In the Returning to Running Postnatal study, they said:
High-impact activity, such as running, is associated with a sudden rise in intra-abdominal pressure (Leitner et al. 2016). It has also been reported that ground reaction forces of between 1.6 and 2.5 times bodyweight can occur when running at a moderate speed of 11 Kilometers/hour (Gottschall and Kram 2005).
Presently, it is unknown if or how much of this is absorbed through the lower limb on impact and therefore it is assumed that some, if not all, of those forces are also transmitted to the pelvic floor.
Return to Running Postnatal–guidelines for medical, health, and fitness professionals. Tom Groom, Grainne Donnelly and Emma Brockwell.
I’ll repeat that…some, if not all, of those forces are also transmitted to the pelvic floor.
Post birth, you have a weaker pelvic floor, especially if you didn’t work those muscles prior to giving birth.
Running can and will make your issues worse if left unresolved.
Tom Groom and his associates said that running is not advisable if you have any of the following symptoms:
- Urinary or fecal incontinence prior to or during running
- Pressure / bulge / dragging in the vagina prior to or during running
- Ongoing or onset of vaginal bleeding (not your menstrual cycle), during or after doing low impact or high impact exercise
- Pelvic pain prior to or during running
Running through these symptoms can make it worse.
TRUST ME. You want to resolve these issues so you can return to running stronger and feel good!
Diaphragm Breathing
Learning how to breathe properly is one of the first steps to take so you can get back running and exercising.
Breathing properly will help stabilize and strengthen your core.
Of course, we all know how to breathe. But, especially as adults, we tend to breathe in our chest which causes shallow breathing. This can also cause pain or strain in your upper body.
The diaphragm is located below your lungs and is the major muscle of respiration. It’s like a muscular wall that separates the lungs from the stomach area.
The diaphragm and the pelvic floor work together. As you breathe through your diaphragm, or belly breath, your pelvic floor contracts and relaxes.
How to Diaphragmatic Breath:
- Find a comfortable position either sitting or lying down on your back.
- Put one hand on your chest and one on your belly or ribs.
- Take a long, slow breath through your nose. As you inhale, your stomach should rise and your ribs expand. Focus on getting air into your ribs and back.
- Exhale through your mouth with your lips pursed together like you’re slowly blowing out a birthday candle.
- Your stomach should rise and fall and your chest should stay still.
- Take a few seconds and repeat 10 times
Diastasis Recti

Another important component to postpartum running is your abdominal muscles.
Diastasis Recti is abdominal separation. (Diastasis=seperation. Recti=rectus abdominis)
It is very common during pregnancy.
Research shows that up to 100% of pregnant women have a diastasis recti of more than 16 millimeters in their final trimester.
Some women may be more prone to separation due to genetics, BMI, weight gain, baby’s birth weight, etc.
As your abdomen expands to accommodate your growing baby, your skin, muscles, and connective tissues stretch out. Your baby needs more space as he or she grows.
You can’t prevent it from happening, but you can try to reduce the severity.
The Linea Alba (in purple below) is the connective tissue joining the two sides of the rectus abdominis muscle (the 6-pack muscle). It runs along your midline from your sternum to pubic bone.
During pregnancy, it relaxes and stretches out and as a result, the distance between your two rectus abdominis muscles (6 pack muscles) increases.
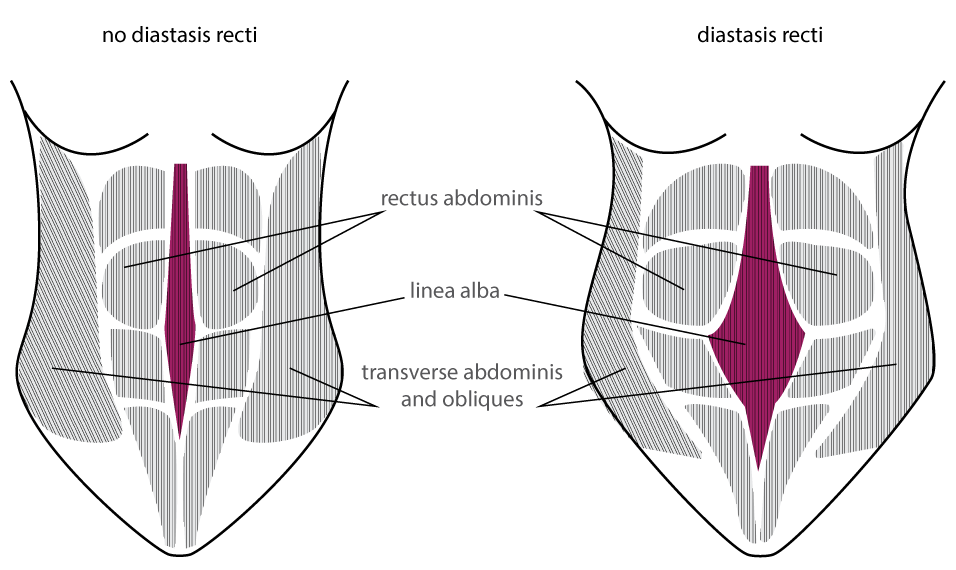
For a lot of women the gap will close naturally in 4-12 weeks postpartum.
For many others it won’t close on it’s own. You will need to do some exercises to help close it.
The good news is, it’s never too late to work on your diastasis recti!
But first, how do you know if you have diastasis recti?
Some common symptoms are:
- Low back pain
- A visible bulge or pooch in your belly (AKA the “mommy pooch”)
- Coning or doming when you contract your ab muscles (like when doing a sit up)
- Poor posture
- Bloating and constipation
- Incontinence
- Feeling of weakness in abs
You might also see “coning or doming” when you do certain exercises or movements like a plank or sit-up. This happens when the abdominal pressure is pushing through the linea alba. You’ll see a raised ridge down your midline.
While pregnant and postpartum you should be mindful of how you get out of bed, etc. Roll to your side and lift up rather than doing a sit up motion to get up.
You can also do a self check:
- Lay on your back and bend your knees with your feet flat on the floor
- Place your fingers just above your belly button with your palm facing you
- Lift your head and neck slightly off the ground and press down with your fingertips
- If you can feel a finger gap between your muscles and it is more than an inch wide, or 2 fingers wide, you may have diastasis recti. The gap can be above your belly button, at your belly button, or below your belly button. The depth of the gap matters as well. That shows how much connective tissue you have left.
Transverse Abdominis
The Transverse Abdominis are muscles are some of the most neglected muscles. I certainly never thought about them prior to having babies.
However, they are SO important for strengthening and stabilizing your core and reducing back pain.
They are located under the obliques in the deep core and wrap around you and help compress your organs.
They’re often referred to as your natural “Spanx”, or like a corset for your organs.
It’s the only abdominal muscle that connects to both the spine and pelvis.
It wraps around the entire pelvis and connects directly to your spine, stabilizing the pelvis and spine together.
It’s essential for stabilizing the pelvis and lower back during movement.
Sorry for repeating myself. But, it’s important. 😜
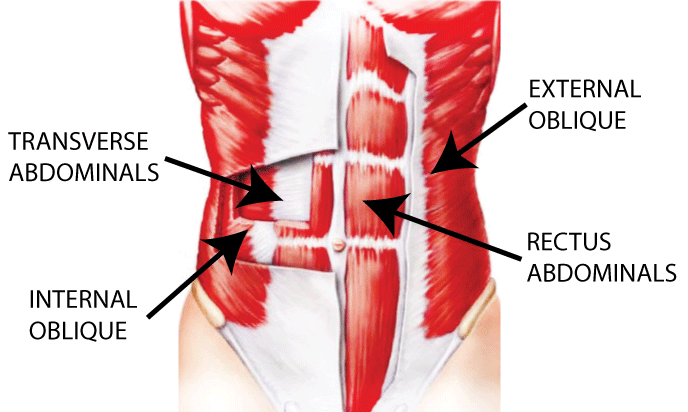
Breathing is the key to activating your Transverse Abdominis.
Shallow breath / chest breathing = poor activation.
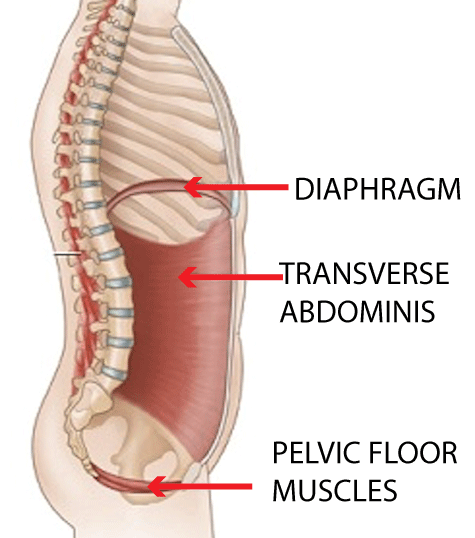
Think of your deep core muscles (transverse abdominis, pelvic floor, and diaphragm) like the walls of a balloon.
They stretch easily but until you fill them with air, they are floppy. They aren’t providing proper stability to the pelvis and spine.
When you inhale, the diaphragm moves downward and the pelvic floor stretches. When you exhale, the diaphragm ascends and the pelvic floor contracts upward.
How to Breathe and Activate your Transverse Abdominis:
- Find a comfortable position. I like laying down on my back.
- Inhale, taking a diaphragmatic breath.
- Right before you exhale, lift and lengthen your pelvic floor (this is not a kegel). Imagine sucking something up through a straw.
- As you exhale, make a ‘SSSSSSS’ sound which will help you keep the air slow and controlled. Don’t be scared to make noise! Your stomach should flatten starting at your lower belly up to your upper belly. Here are some useful cues:
- Imagine a rolling pin rolling from your lower belly to your upper belly pushing all the air out
- Imagine zipping up a tight jacket
- Imagine that your cinching up a corset
- Imagine bringing your hip bones closer together, your obliques to touch, your ribs closer together
- Belly button in and up
- Do not hold your breath or suck in your spine!
- Once you’ve exhaled, relax your pelvic floor. Take a few seconds and repeat.
One more tip that helped me recognize if I’m activating my transverse abdominis was to lay down and place my hand 1″ in from my hip bone and 1″ down from my hip bone. When activated, you should feel the muscle tighten.
Aside from breathing exercises, let’s go over a few other deep core exercises you can do as your prepare to run!
Deep Core Exercises
Heel Slides
First, activate your TVA. Inhale, exhale, lift your pelvic floor with the “sssss” breath. Wrap your TVA in.
Keep your heel in contact with the ground as you slowly extend one leg. Exhale to extend your leg, inhale to slide your heel back in.
Glute Bridge Marching
First, activate your TVA. Inhale, exhale, lift your pelvic floor with the “sssss” breath. Wrap your TVA in. Think about putting on a tight pair of jeans, bringing those hip bones closer together.
Lift your glutes up into bridge position. Lift one leg, bring back down and alternate. Try to keep you pelvis/hips square. Don’t let one side dip down.
Toe Taps
First, activate your TVA. Inhale, exhale, lift your pelvic floor with the “sssss” breath. Wrap your TVA in.
Bring your legs up into table top position and slowly tap one foot down to the ground and bring it back up. Alternate sides. Keep you TVA turned on and continue breathing through this movement.
Knee Drops
First, activate your TVA. Inhale, exhale, lift your pelvic floor with the “sssss” breath. Wrap your TVA in.
Slowly drop one knee to the side. Control the movement and be sure you keep you TVA turned on and continue breathing.
Frog Pose – relaxing your pelvic floor
This exercise to meant to RELAX your pelvic floor. You are not contracting. It’s a modified child’s pose. Try to imagine your hips WIDENING as you relax and breathe.
Position your body with you forehead on the ground, arms relaxed infront, and butt in the air (kind of like how babies like to sleep). Your butt should be past 90 degrees.
Completely relax into the ground.
Don’t brace any muscle in your body.
Get heavy.
Mentally focus and envision releasing your pelvic floor. Feel your pelvic floor and hips widen and stretch out.
3. Postpartum Assessment
Load and Impact Assessment
As mentioned above, when you run, the impact on your body is up to 2 times your bodyweight.
In the return to running study ( 2019 study), they provided some exercises to assess if your body is ready to return to running.
You need to be able to do the following without pain, heaviness, dragging, or incontinence.
- Walking for 30 minutes
- Single leg balance – 10 seconds
- Single leg squat – 10 reps each leg
- Jog in place for 1 minute
- Forward bounds – 10 reps
- Hop in place – 10 reps each leg
- Single leg ‘running man’ (opposite arm and hip flexion/extension (bent knee) – 10 reps each side
If you do experience any symptoms or are unable to complete any of the exercises, that’s okay!
It can help identify what you need to work on or strengthen.
Strength Assessment
These exercises also come from the 2019 study
The purpose of this assessment is to determine if the key muscle groups are prepared for running.
Aim for 20 reps of each test.
- Single leg calf raise
- Single leg bridge
- Single leg sit to stand
- Side lying abduction
Any weaknesses found while doing these exercises can also help identify where strength work is needed most!
4. Postpartum Running Form
Your body goes through a lot changes during pregnancy!
- Your center of gravity changes as your belly grows, which can cause your hips and feet to rotate outward in order to increase your base of support. This can can cause tight and weakened hips because you’ve shortening the hip muscles. You will need to strengthen your gluteus medius and minimus to combat this.
- Increased ankle tightness and lack of flexibility
- Arched back or poor posture
All of these changes can affect your running form postpartum.
I highly recommend running outside, barefoot, and recording your run from the side, front, and back. This will give you an idea of what you’re currently doing, and what you need to work on.
So let’s get into what you want to look for as you analyze your run!

- Alignment
- Align your shoulders, hips, knees and toes together
- Eye Gaze. Look about 15-20 feet ahead of you.
- Ears aligned with your shoulders.
- Relax your shoulders. Don’t shrug those shoulders!
- Glute Activation
- Apply the S-pose. This means you’ll be in a slight mini squat which will help you get good glute activation. Remember, your glutes muscles are large! They should be taking most of the force. The s-pose will help with this.
- You should feel your glutes activate every time your foot hits the ground. Now, this doesn’t mean it will feel like you’re doing a squat or deadlift – not that intense, but you should feel them working.
- Try doing some glute activation drills. We often have sleepy glutes from sitting too much.
- Think, light and soft feet
- Arm Drive and Obliques (pendulum motion)
- Your left leg and right arm move together; your right leg and left arm move together
- This will propel you forward and help increase your cadence
- Imagine a line going down the center of your body; try not to let your arms cross that line
- Also, be sure not to tense up your hands in fists, this can cause you to tense up in your upper body too
- Falling / Forward Lean
- Let gravity do the work! Lean forward from your ankles
- The faster you run, the more you lean
- Do a fall forward drill to help get the feel of this
- Your posture should be tall, but not straight up and down
- Fast Feet
- Keep your cadence high (170-180 steps per minute). This can help reduce the load to your muscles and body by using gravity to keep you moving forward.
- Feet should land underneath your hips.
- Avoid overstriding. Overstriding is when your foot lands in front of you. This is like applying the breaks and will require you to work harder to move forward! Momentum is your friend when running.
- Heel striking is somewhat controversial and I admit, it’s something my husband and I have argued about over the years as he noticed I was heel striking. haha… however, after having a pretty significant injury and going through a whole program to get me running again, I have changed my tune. Mid-striking is optimal. Heel striking can increase the impact of hitting the ground which can lead to injury. It also increases the contact time your on the ground which can slow you down.
5. Preparing to Run
In the U.S. you will have an appointment with your OBGYN at 6 weeks postpartum. If you’ve healed well, this is usually when you’re given the green light to exercise and do anything and everything you did prior to pregnancy.
However, you don’t have to wait until that appointment to start preparing for running and exercise. Of course this will vary person to person, but generally, it’s good to start walking and doing LIGHT pelvic floor exercises.
Walking
One of the tests mentioned above was being able to walk for 30 minutes without pain, heaviness, dragging, or incontinence.
This is something you can start to work on pretty early postpartum.

Walking was always something I looked forward to in those early postpartum days. I always get cabin fever staying at home so much so it was nice to get outside and do something.
Walking will help you build up your strength and endurance.
It’s also great for your mental health!
During the first 1-4 weeks, you want to gradually increase the time you’re walking.
For example, week one could be 2-3 minute walk and rest. Twice daily. That’s it!
By week 4 you could be up to something like :
15 minute walk / 5 minute rest / 10 minute walk / 5 minute rest
After 6 weeks you can add in more low impact cardio like swimming, biking, and the elliptical.
Always listen to your body and if you feel like it’s too much, stop or scale back.
Strength Training
Starting at 6 weeks, begin some strength training.
A lot of runners have weak hips – even those who were never pregnant so it’s important to work on strengthening your glute muscles postpartum.

Step-ups, squats, deadlifts, bulgarian split squats are all great exercises to help strengthen your glutes.
Single leg and balance/stability exercises are also great.
Of course, you’ll want to include strength workouts for your whole body.
Running is a full body workout.
Everything is connected in your body so if one muscle is weak, it can cause extra stress or compensation on other muscles.
Strength training will help prevent injury, make you stronger, faster, and give you some nice looking muscles too. 😁
Learn more about strength training here.
6. Postpartum Obstacles: Other things to consider
Posture
The strength of your core can have an affect on your posture and visa versa. As new moms, it’s easy to fall into some bad habits with posture since you have a weakened core, are holding a baby, breastfeeding, etc.
When you’re standing, pay attention to your posture. Are you pushing your hips forward? Arching your back? You want to work towards a neutral spine alignment shown in the image below.
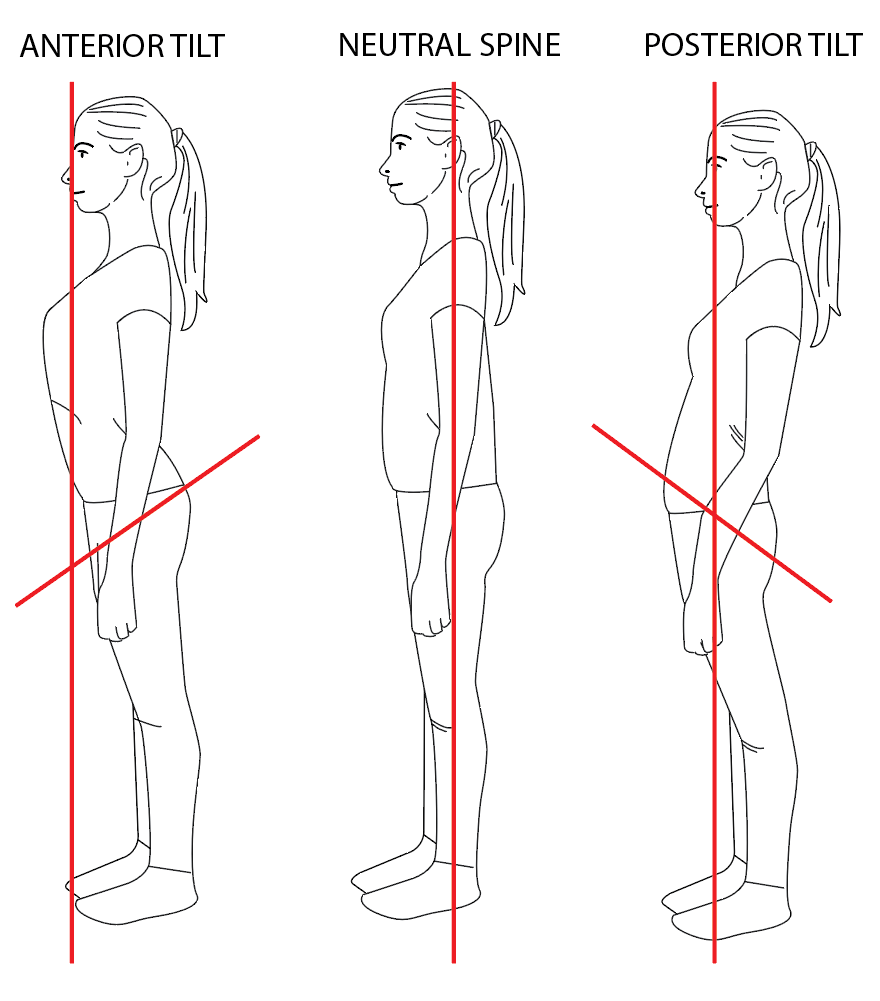
Anterior Pelvic Tilt is when push your butt back, arch your back, and push your chest forward. This is very common with pregnant women. You may have tight hip flexors, tight back muscles, weak hamstrings, and abdominal weakness
Posterior Pelvic Tilt is when you push your hips forward so your rib cage sits behind your pelvis. You may have tight hamstrings, tight back muscles, weak abdominals and weak hip flexors.
Both of these postures can cause back, hip, knee, and neck pain. Not ideal!
Try to keep your pelvis, ribcage, shoulders, head stacked on top of each other. I know, it’s hard when you’re holding babies, breastfeeding, etc. but try to be more aware of it.
Engage your core as much as possible as you lift and hold your baby.
Sleep
Obviously this is something you will be lacking as a new mother. Try to rest as much as possible. Ask for help where you can.
If you had a terrible nights sleep, consider skipping your run or reducing the time so you can recover.
Communicate with your spouse or partner about the importance of exercise for you so you can get help in this area. They can be pretty oblivious sometimes so it’s important to be direct. 😉

Nutrition

Drink lots of water and try to eat as many whole foods as possible.
Whole foods = not packaged or processed.
When you’re sleep deprived, you’ll probably crave more sugar, but it’s important to give your body nutrients so you can have energy. Especially if you are also breastfeeding.
However, no need to eliminate sugar completely as long as you’re also eating fruits, veggies, and protein. If you need help with this, I’m happy to help. Find out more here.
Breastfeeding
A common myth I heard when I first has my baby was that if I run or exercise too much, I’ll lose my milk supply. However, there are studies out there that show there is no difference in milk production or milk composition for mamas who exercise vs. mamas who don’t.
If you are doing a very intense run or workout, you may have some lactic acid in your milk, but most studies have found that does not affect the baby accepting the milk or not.
Bottom line. Make sure you are drinking and eating more to keep up your milk supply as exercise may put you in a calorie deficit.

Feet
You’re feet can change a lot during pregnancy. Some women report going up a size or 1/2 a size or having a wider foot postpartum.
A number of women also experience pain in the arch (plantar fasciitis) during pregnancy due to the changes of your center of gravity, pointing your toes more outward while walking and standing. That can put additional pressure on the arch.
First, it’s important to make sure you have the right footwear. If you’re shoes feel tight or uncomfortable, look into getting new shoes. You might also find that the model of shoe you preferred pre-pregnancy doesn’t work as well postpartum.
Second, work on strengthening and activating the muscles in your feet and retraining them so they are prepared for running.
Obviously your feet are an important component to running, but it’s something we often neglect.
7. Conclusion
Let’s summarize the general guideline to return to running:
- Prior to 6 weeks, start doing some light deep core/pelvic floor work.
- Prior to 6 weeks, starting walking. Ease into this and start small.
- At 6 weeks, go to your OBGYN to get assessed. If all is well, they will give you the green light to do anything and everything.
- At 6 weeks, before doing anything and everything, go to a pelvic floor specialist to be assessed and given specific guidance for your body.
- 6-12 weeks, continue doing core/pelvic floor work as well as full body strength training, head to toe. Listen to your body and back off intensity if needed.
- 12-18 weeks, if all is well, start a couch to 5k program or something similar to begin running. As I’ve stressed throughout this article, everyone is different. You could be ready to run earlier or even later. Work with a pelvic PT, your doctor, and be your own advocate to help determine what’s best for you.
Listen to your body as you start running again. Ease back into it.
Have fun and don’t put pressure on yourself.
Allow yourself to properly recover when you get back to running – you might need more time than normal to recover between runs.
Don’t ignore any running niggles that come up. Give them attention and treatment rather than running through them.
Go see a pelvic floor therapist especially if you have any of these symptoms:
- heaviness or pressure in your vagina or rectum
- leakage or incontinence
- painful sex
I know this is cliche, but enjoy this time with your little baby. It really does go SO FAST. You will have plenty of time to get back into running and racing.
You can come back even stronger and faster than you were before. 💪🏼
Lastly, if you have any questions, comment below or email me. christyewingfitness@gmail.com
Please share this if you found it useful.
I’d also love for you to join my mailing list so you can be the first to know of any new articles coming out. Sign up below!
Thank you for being here and reading this. I truly hope it helps and you feel more prepared, confident, and hopeful about running postpartum!
xoxo,
Christy


