Nutrition during pregnancy can be tricky. One one hand, you want to provide your baby and yourself with the best, but on the other hand, you’re dealing with extreme fatigue, nausea, heartburn, food aversions, and cravings!
I’m currently on my 4th pregnancy and have coached a handful of prenatal clients through this time. I’ve learned a lot of what works and what doesn’t work during pregnancy and I hope you can learn a lot from this article.

I’m going to take you through all 3 trimesters and go over how you can approach nutrition throughout your pregnancy. Here’s a quick overview:
- 1st Trimester
- The Building Blocks of Nutrition
- Building Habits
- Nutrition Considerations During Pregnancy
- 2nd Trimester
- Meal Frequency
- 3rd Trimester
- Relief For An Upset Stomach
1st Trimester
People love to say, “Now that you’re pregnant, you’re eating for two, right?”
There is some truth to it, but it doesn’t mean what most people think.
The Academy of Nutrition and Dietetics said that women generally don’t require additional calories in the first trimester1. Your daily calorie requirements do increase as your pregnancy progresses:
- 1st Trimester: no additional calories needed
- 2nd Trimester: about 340 more calories
- 3rd Trimester: about 450 more calories
- Breastfeeding: about 500 more calories
I share this for informational purposes. I don’t recommend that you count calories during pregnancy.
I do recommend focusing on eating high-quality, whole, nourishing foods.
The extra stress of measuring, weighing, and counting calories can be too much in an already somewhat stressful time. Especially if you are suffering from nausea, food aversions, etc. A lot of woman are just in survival mode during the first trimester!
I want you to focus on developing good habits instead. The next several sections are “building blocks” to a well-fueled pregnancy for you and your baby.
Building Blocks of Nutrition
Protein

- Protein is essential for building and maintaining muscle. It is the perfect pair to your strength training routine.
- Protein will also help you feel full and satiated which can help with morning sickness. An empty stomach can make nausea worse.
- Protein is also necessary for building structural proteins that will be the building blocks of your baby–collagen, elastin, muscle, tendons, enzymes.
Fruits and Vegetables

- Not only are they delicious, but fruits and vegetables are packed with vitamins, micro-nutrients, and antioxidants that will improve your overall health and help you feel better.
- They’re also a great source of fiber which will help reduce constipation which can help prevent unpleasant pregnancy issues like hemorrhoids.
- Fiber will also help you to feel full and satiated during meals which can prevent overeating.
Dietary Fats

Fat can get a bad wrap, but they are essential and necessary for your health!
- Omega-3 and omega-6 fatty acids are good for brain function and the structure of your cell walls.
- Fats also promote healthy hormone levels.
- They help keep you more satisfied after meals.
- They are essential for your baby to develop optimal brain and eye health.
Most people are able to get enough omega-6 fatty acids from their diet, but don’t get enough omega-3 fatty acids (DHA and EPA). You can also increase your omega 3-fatty acids by eating fish, walnuts, hemp seed butter, hemp seeds, and fish oil supplements.
Whole Carbs

Carbs are also often given a bad wrap. However, just like fats and protein, they are essential!
- They give you energy (which is SO needed during pregnancy!!), promote healthy hormone levels, and replenish the glycogen stores that become depleted during intense exercise.
- Carbohydrates are FUEL for your body and give you energy which is very much needed especially during pregnancy!
Try to focus on nutrient-dense carb choices rather than heavily processed foods. Examples of nutrient-dense carbs are oatmeal, rice, oat bran, quinoa, fruits, and veggies.
Most nutrient-dense foods have fewer calories and are filled with micronutrients.
You don’t need to completely avoid less nutrient-dense carbs (think crackers, white bread, cookies, chips, etc), but let the main focus be on nutrient-dense.
Hydration

Water is essential for everyone, but especially pregnant women.
Dehydration can cause headaches, lethargy, difficulty concentrations, and can disrupt bodily functions. All of these can be problematic during pregnancy.
During pregnancy, the body’s blood volume slowly increases by 40-50%, meaning that maintaining proper hydration levels becomes even more important.
The National Academies of Sciences, Engineering, and Medicine recommends pregnant women consume 101 oz (3 liters) of water daily2.
Serving Sizes
Since you aren’t “counting calories” or measuring or weighing your food, how will you know the proper serving sizes?
There are 2 methods that I like to use. The first is the “hand portion” method.
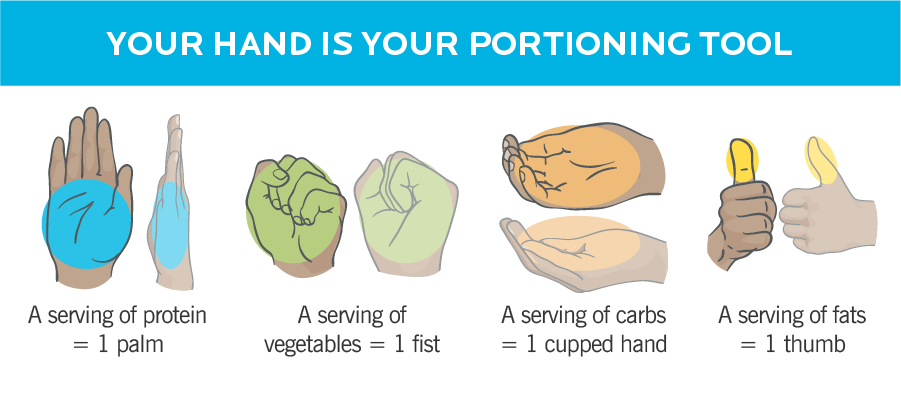
- 1 serving of protein = size and thickness of your palm
- 1 serving of veggies/fruit = size of your fist
- 1 serving of carbs = size of your cupped hand
- 1 serving of fat = size of your thumb
Another method is the plate method. Each meal should fit on a normal-sized plate. 1/2 the plate is veggies, 1/4 of the plate is a protein, and the rest is carbs and fat. Have 2-3 snacks that’s a fruit, veggie, or protein and is the size of your fist.
Meal Frequency
This is really up to each individual. It depends on your personal preference, hunger, and schedule.
Some prefer more than 3 meals a day, some prefer less. Do what works best for you and keep in mind that this may change throughout pregnancy and that’s okay. By the 3rd trimester when your stomach is being crowded by baby, you might prefer several small meals rather than 3 bigger meals.
The most important thing is to listen to your body and eat when you’re hungry, stop when you’re satisfied.
Nausea
In my opinion, nausea is the worst symptom during pregnancy! I’ve suffered with “morning sickness” which is actually all day and night sickness with all 4 of my pregnancies.
It’s terrible, but hopefully it lessens as your pregnancy continues or goes away completely. There are things you can do to help ease the nausea, but I recommend talking to your doctor. Especially if it’s interfering with your ability to eat and/or stay hydrated.
You might benefit from eating small meals or snacks even before you feel hungry. It helps prevent dips in blood sugar, which is linked to nausea. Some people might even benefit from eating something small in the middle of the night if you get up to pee. This may help combat next-morning nausea.
Protein is ideal to help you fill full, but do what you can. Opt for bland foods vs. spicy or overly fragrant foods!
Another tip is to take your multivitamin or prenatal after a meal, not on an empty stomach.
Take small sips of water throughout the day to help you feel hydrated.
Building Habits
Now that we’ve gone over the ‘building blocks of good nutrition’, let’s dive into HOW we can apply everything. This can be the most challenging part!
A 2012 scientific review from experts at the University College London’s Health Behaviour Research Centre3 shows that habit formation is integral to making lasting changes that, in the end, happen automatically and without thought, even when motivation wanes.
If you’ve read Atomic Habits, this idea won’t be new to you.
Try to practice 1 new, manageable habit at a time until it feels natural or until you’ve been at least 80% consistent for 2 weeks. After that, try adding a new habit into the mix. Trying to change too many things at once can be very overwhelming or unsustainable which can cause you to quit or give up.
That’s why so many fad diets fail. They’re asking you to change everything at once–how you eat, when you eat, how much you eat, where you shop, etc.
A habit-based approach is much more sustainable, realistic, and effective. It will help you be consistent, which is one of the most important things when it comes to building habits.
Think of these habits as building blocks or bricks to a healthy diet. Each new habit is building on top of the next, creating a solid foundation.

Start with one habit, practice it for 2 weeks, tracking your consistency. Try to be 80% consistent with this habit before implementing the next habit. Some habits might take more time, and that’s okay.
Below are 8 healthy habits you can try to master:
1. Take at least 20 minutes to eat a meal and at least 10 minutes to eat a snack

Slow down and be more mindful when you’re eating. Avoid distractions like the TV, phone, computer, etc.
This will help you enjoy your food more, feel more satisfied, and it’ll help you tune into your body more.
Slowing down allows your stomach to signal to your brain when you’re satisfied or full so you can stop eating before you are uncomfortably full. Being too full can make nausea worse, heartburn flare up, or just be very uncomfortable!
I know it’s hard to do this as a busy mom. It seems like we’re always eating on the go or as fast as we can so we can get to the next task or before we’re interrupted by a screaming child.
Do what you can and try your best. Here are some more tips to implement eating slowly:
- Set a timer on your phone to give you an idea of how slowly or quickly you’re actually eating.
- Focus on the appearance, smell, taste, and texture of your food.
- Take smaller bites of food (you can even use a kiddie utensil).
- Put your fork down between bites.
- Chew your food until it’s almost liquid.
- Take sips of water between bites.
- Engage in conversation with your dinner companion.
- Pause to check in with yourself and your hunger cues when your plate is one-fourth, one-half, and three-fourths empty.
If 20 minutes for a meal and 10 minutes for a snack feels really hard, cut the numbers down to one that feels realistic. Maybe that’s 12 minutes and 6 minutes. You can start there and work up to 20 and 10.
2. Stop eating when you’re satisfied, not stuffed.
This one can be hard, especially if you’re eating something that’s really good.
It can also be hard to determine when you’re satisfied vs. stuffed. Eating slowly will help with this.
If you start to feel discomfort or pressure in your abdomen, you’ve gone beyond satisfied. Keep listening to your fullness cues and over time, this habit will get easier.
Here are some tips to help with this:
- Eliminate distractions during meals. No phone, no TV, no computer. This will help you tune into what you’re eating and recognize your fullness cues more easily.
- Pay close attention to the portion sizes listed at the beginning of this guide when you’re dishing food onto your plate.
- If you struggle with portion sizes, use a smaller plate to trick your brain into thinking you’re eating more.
- When your plate is ¼, ½, ¾ empty, practice the “stop and savor” moments. Be mindful of what is in your mouth, how quickly you fill your fork, how well you are chewing your food.
Notice the flavors, smells, textures, tastes, etc. Have you adequately chewed and swallowed the previous bite before scooping another bite?
3. Eat protein with every meal or snack.

Protein is filling, satisfying, and vital to maintaining a healthy body.
Proteins, composed of amino acids, are literally the building blocks of life. They make and grow every tissue in the body.
They are critical for muscle repair and growth, and even make up your body’s supply of hormones, neurotransmitters, and antibodies. Your body needs protein to grow and nurture a baby.
To get adequate protein, eat a whole serving (size of your palm) of a food rich in protein with every meal and either ½ a serving of a food rich in protein or whole serving of a food that contains a moderate amount protein with every snack.
What is “rich in protein” and “moderate amount of protein”?
Animal sources like chicken, beef, salmon, eggs, turkey, plain greek yogurt, cottage cheese are all protein rich. There are many plant-based foods like nut butters, legumes that provide a moderate amount of protein. Good sources of protein will have at least 10g of protein for every 100 calories.
Here are some tips to help you get more protein into your diet:
- When planning your meal/snack, consider the protein source first and then build the meal around the protein source. Make protein the star of every meal.
- Add a scoop of protein powder to foods your already consuming like oatmeal and smoothies.
- Choose high-protein versions of your favorite foods. For example, Greek yogurt instead of plain yogurt.
- Determine where you can swap higher-protein foods for lower-protein foods.
- Cook protein-rich foods in large batches so you have plenty on hand throughout the week.
- Increase the portion size of what you’re already eating. For example, if you’re eating 4 oz of chicken, increase it to 6 oz or 8 oz.
4. Eat a serving of veggies or fruits with every meal or snack, or five servings of veggies and fruits per day.

Fruits and vegetables are fibrous, filling, and full of vitamins, minerals, and antioxidants to help keep you healthy.
Plus, relative to their volume, they are low in calorie so they will fill you up and satisfy you with fewer calories than other foods. For example, ONE POUND of watermelon is only 138 calories.
2 cups of broccoli is 62 calories. In contrast, 2 cups of pretzel sticks is about 350 calories.
Enjoy a variety of fruits and veggies. Here are a few examples:
- Green: spinach, kale, kiwi, broccoli, green apple, asparagus, zucchini, green pepper, brussel sprout
- Red: grapefruit, watermelon, red pepper, cherry, strawberry, radish
- Blue/Purple: eggplant, cabbage, plum, blueberry, black olive
- Yellow/Orange: yellow pepper, pineapple, butternut squash, cantaloupe, pumpkin
- White/ Beige: banana, mushroom, onion, potato, cauliflower, jicama, garlic
Aim to eat 5 servings of fruits and vegetables per day or eating fruits and vegetables with every meal/snack.
Here are some tips to get more protein and veggies in your diet:
- Fruit and veggie smoothies
- A big salad for one meal
- Buy pre-chopped or packaged fruits to help save time
- Have frozen fruits and veggies on hand when you don’t have any fresh options
- Add fruits of veggies to foods that you’re already eating. For example, spinach to your eggs, blueberries to your oatmeal, carrots and onions to your soup, etc.
- Use veggies as a substitute for other foods. For example, zucchini noodles instead of spaghetti.
- Cook veggies in large batches to have ready-to-eat veggies on hand.
- Use a salad chopper to chop your salad veggies into small pieces. This can make salads much more palatable for people who don’t normally love salads.
5. Eat high-quality dietary fat with every meal or snack.
Dietary fats are important for balancing blood sugar, feeling more satiated, reducing cravings, helping you feel fuller longer, and helping you absorb fat-soluble nutrients.
Good sources of healthful fats include nuts, seeds, olives, avocado, coconut, fatty fish, grass-fed or pastured animal products (meat, cheese, butter yogurt),
Omega-3 fatty acids from fish like salmon or in a high-quality supplement have been shown to decrease inflammation, lower risk for chronic disease, and improve immune functioning.
Fats are calorically dense, to paying attention to serving size is important. A serving size is roughly the size of your thumb.
Aim to have 1 serving of dietary fat with every meal and ½ serving with every snack.
Here are some tips to help you get enough high-quality dietary fat with each meal:
- If you normally eat egg whites, add or substitute 1-2 whole eggs
- Use coconut oil, avocado oil, real butter, or ghee when cooking.
- Add a drizzle of olive oil or an oil-based dressing to your salsa or veggies.
- Add a serving of nuts to your salad, greek yogurt, oatmeal, or stir-fry. Or spread a tablespoon or 2 of nut butter on your fruits or veggies.
6. Eat whole, unprocessed, or minimally processed carbohydrates in place of refined carbohydrates.

It’s easy to consume way more carbs than your body needs when the source is from a heavily processed food. Whole carbs including fruits, veggies, potatoes, oats, rice, and quinoa are dense in nutrients and higher in fiber. Aim to choose whole carbs 80% of the time. You don’t need to cut out processed foods completely.
Here are some tips to incorporate whole or minimally processed carbs into your diet:
- Make large batches of your favorite whole carb like rice, quinoa, or sweet potatoes so you always have them on hand to add to your meal.
- Swap out highly processed carbs for their minimally processed relatives like whole potatoes instead potato chips.
- Choose whole grain options like whole grain pasta, bread, or tortillas in place of their white varieties.
7. Drink half your body weight in ounces of water per day
Dehydration affects your digestion , cognition, skin health, body temperature regulation, and your performance in the gym.
It’s recommended that pregnant women should consume 101 ounces of water per day. When breastfeeding, the requirement goes up to 128 ounces. But remember, this is just an average, and your individual needs may vary. Also, fluid-filled foods like soups and oatmeal count towards those totals.
Here are some tips to increase your water intake:
- If you find plain water boring, liven things up with unsweetened sparkling water or by adding lemon, lime, cucumber, or mint to your water. True Lemon has some good flavored water packets as well.
- Set a timer for every hour. When the times goes off, stand up, stretch, and take a few big gulps of water. (aim for 4-6 oz)
- Chug a big glass of water first thing in the morning. (I don’t recommend this if you’re suffering from nausea)
- Drink through a large straw. You’ll drink more without noticing.
- Have water on hand whenever possible. (water bottle)
8. Take your supplements as directed.
We’ll dive into this deeper in the supplements section, but here are some tips to help you get into the habit of taking them regularly:
- Get a pill organizer so they’re already portioned out each day.
- Pair your supplements with another morning habit like brushing your teeth or after breakfast.
- Try taking supplements mid-meal, especially if they make you feel nauseated.
Nutrition Considerations During Pregnancy
Food to Eat in Moderation
I don’t believe that you should avoid any food 100%. (Unless you’re allergic or sensitive, or it can be harmful during pregnancy). I recommend approaching less nutrient dense foods with an “everything in moderation” approach.
Focusing on the healthy habits we outlined above will help ensure that you’re eating minimally processed, nutrient-dense foods most of the time, which leaves some (but not too much) room for the following foods:
Highly Processed Foods
If it comes in a bag or box from the middle aisles of the grocery store and contains a lengthy list of hard to pronounce ingredients, it probably shouldn’t be a staple in your diet.
These foods tend to be low in nutrient density, meaning they are high in calories and low in vitamins and minerals. Examples are crackers, chips, cookies, cereal, and candy.

Caffeine
High caffeine consumption can increase the risk of miscarriage, reduced birth weight, and stillbirth.
The amount of caffeine linked to these problems is not definitive in the research, but the American College of Obstetricians and Gynecologists4 recommends limiting consumption to 200 milligrams, which is the equivalent of 12 oz or 2 cups of caffeinated coffee per day, when pregnant.
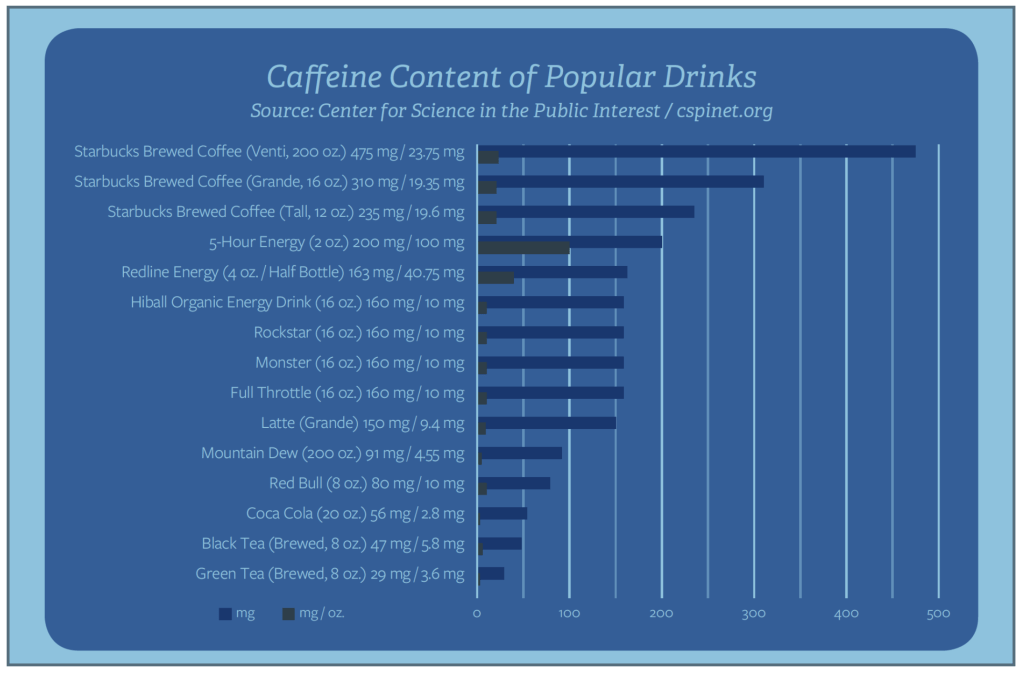
Sugary Beverages
Sodas, energy drinks, fancy coffee drinks are loaded with empty calories that provide virtually no nutrition and don’t satisfy hunger.
Keep this in mind as you choose your beverages! They don’t need to be avoided completely, but I’d recommend having them in moderation or special occasions.

Are there foods you should avoid completely?
The only foods you need to “avoid” are foods to which you’re allergic or sensitive to and foods that could be harmful to your baby. Check with your doctor for a list of those foods.
Alcohol
Beer, wine, and spirits can be detrimental to a developing fetus and can result in fetal alcohol syndrome.5 According to the American Congress of Obstetricians and Gynecologists, no amount of alcohol is known to be safe during pregnancy.
Foods Linked to Listeriosis
Listeriosis is a serious infection caused by eating foods that contain the bacteria Listeriosis monocytogenes. It can lead to miscarriage, stillbirth, and other serious health problems. Listeria can occasionally be found in lunch meats, processed meats, hot dogs, and some seafood.
Listeriosis guidelines vary per country, so talk to your doctor before ruling out these foods. A common one talked about is lunch meat. I really crave turkey sandwiches during pregnancy so I just heat the turkey up first.

Raw or Undercooked Proteins
Avoid sushi, unpasteurized eggs, raw cookie dough or cake batter, runny eggs, raw seafood, and rare cuts of meat due to the risk of listeriosis. Use a thermometer to ensure that your meats are cooked through to the middle. It is also best to avoid raw milk and cheeses, including Brie and feta, that are made with unpasteurized dairy.
Raw Vegetable Sprouts
You can eat veggie sprouts during pregnancy, just not when they are in their raw form. Some varieties carry a risk of foodborne illness when consumed raw.
If they are fully cooked, however, any potential bacteria is killed and they are considered safe for consumption by pregnant women.
Foods Exposed to BPA
BPA is a compound in many household items, including plastic water bottles and the lining of tin cans. Due to its hormonal properties, large doses consumed by pregnant women have been linked with poor fetal health outcomes. Opt for BPA-free water bottles and rinse any canned fruits or veggies in water.
Foods Contaminated with Lead and Mercury
These two heavy metals can find their way into your diets through a number of sources and can disrupt the neurological development of the fetus, causing neurological disorders and delays. To avoid lead consumption, do your best to make sure that any supplements that you take or plan to take during pregnancy do not contain lead. This is tough because supplements are largely unregulated, so it is best to diligently research brands or ask your health care practitioner for a recommendation to reduce your chance of contamination.
When choosing a water bottle, look for one labeled lead-free since some plastics can also contain lead. If your home has old, lead pipes, lead can also leach from them into your tap water. If you’re concerned about your tap water, you can have it tested. To be extra cautious, now may be the time to splurge on a water purification system for your home. Speak with your healthcare practitioner to help determine the safety of your drinking water.
Mercury is often found in older, larger fish such as swordfish, shark, king mackerel, and tilefish, and in some fish oil supplements. Tuna also contains some mercury. Limit yourself to no more than two cans per week and choose chunk light instead of white tuna.
The Environmental Protection Agency states that it is safe for pregnant women to eat as much as eight to 12 ounces of fish or seafood low in mercury per week (or approximately two meals).6
Safer selections include shrimp, salmon, pollock, catfish, anchovies, and trout. When shopping for fish oil supplements, research the brands carefully to ensure that the ingredients used are of high quality. Salmon, anchovy, and sardine oils are great choices. Look for “molecularly distilled and filtered” on any labels to ensure that all heavy metals have been removed.
2nd Trimester

Phew! Got past the bulk of information in the 1st Trimester section. I hope you’re still here.
Back in Trimester 1, we discussed the building blocks of good nutrition during pregnancy, as well as some healthy habits you can work on incorporating into your routine.
As you continue to practice and master theses things, there are only a few small changes to keep in mind as your pregnancy progresses, most notably in regard to an increase in caloric requirements.
According to the recommendations from the Academy of Nutrition and Dietetics, women generally do not require additional calories in the first trimester. Daily calorie requirements will increase above baseline needs by about 340 calories in the second trimester.
That said, don’t stress about exact numbers. Like I mentioned earlier, instead of counting calories, your best bet is to continue focusing on the habits outlined in the sections above and simply let your hunger and fullness cues be your guide.
Your body naturally “knows” that it needs some extra calories as your pregnancy progresses. If you have any concerns about your weight gain (or lack thereof), talk to your doctor.
Another nutritional need that changes during trimester two is the amount of iron you require.
Adequate iron intake is necessary to make hemoglobin (the part of your red blood cells that carries oxygen), and as your blood volume increases along with the size of your baby and placenta, your body needs more iron.
Prenatal vitamins contain iron, but it’s still possible to become anemic in pregnancy.
If your fatigue doesn’t clear up in your second trimester (many pregnancy symptoms ease up during this time), or you feel exhausted or weak, talk to your doctor about your iron levels and get blood work done to determine if you have anemia.
It may be necessary to take an iron supplement. (Don’t take your iron supplements at the same time that you ingest any calcium-containing supplements or foods. Calcium can reduce iron absorption.)
One thing I want to note is that many iron supplements can cause constipation. If this happens to you, please discuss with your doctor for some suggestions to help with this. Remember, constipation can cause a lot of strain in the pelvic floor and should be avoided as much as possible.
Finally, you may also want to talk to your doctor about supplementing with additional calcium and magnesium during your second trimester as your baby’s bones are hardening and may start robbing you of these minerals. If you experience twitching or cramping, this may be a sign that supplementation could help.
Meal Frequency
Meal frequency is going to depend on your schedule, preferences, and hunger.
Many women do really well eating something every three or four hours. That might mean eating four meals a day (using the portion sizes we outlined in the 1st Trimester section), or three meals and a couple of snacks per day.
Your preferred meal frequency may change throughout your pregnancy. Both hunger levels and the amount of food that your stomach can comfortably hold will change throughout pregnancy.
You may find that, as your pregnancy progresses, you feel better eating smaller, more frequent meals than you were eating prior to conception or during your first trimester.
The most important thing here is to listen to your body: eat when you’re hungry, stop when you’re satisfied, and pay attention to how your body responds.
3rd Trimester
We’re cruising now! Already into the 3rd trimester. 😉
During your third trimester, your nutrition goals will be the same as they were during the rest of your pregnancy. Continue practicing the core nutrition habits to ensure that you’re getting enough protein, vegetables, fruits, grains, healthy fats, water, and plenty of good nutrition for your little one.
During this trimester, you may notice fluctuations in your appetite.
At this point, you should be consuming about 450 extra calories per day to support your pregnancy and growing baby, according to the Academy of Nutrition and Dietetics.
Again, don’t stress about exact numbers. If you pay attention to your hunger and satiety cues, and your doctor doesn’t raise any concerns about your weight, you should be fine.
Some days, you may notice that you have a bigger appetite. On others, you may notice that you have little interest in food. Your growing belly may cause discomfort that limits your appetite. You may start to feel full sooner than you used to. If this is the case, try to eat small, frequent meals, but don’t stress if you’re just not as hungry as you have been in the past.
As long as your doctor is happy with your health and your baby’s progress everything is fine.
This is also the trimester in which you will likely notice the biggest weight increases.
But, don’t worry or stress, this is very good news!
Your baby is growing, and you’re getting closer to meeting your baby! Even if you’re not tracking your weight, your medical team is. Your doctor or midwife will record your weight at your bi-weekly appointments. I honestly don’t pay attention to it and my doctor’s office weighs me in kilograms, which I’m not familiar with since I am used to pounds. So, I see the weight, but don’t really know what it means.

The goal is to see slight increases in weight at every check-in. Just keep listening to your body’s cues. Eat when you’re hungry, stop when you’re satisfied, and don’t stress. Also, every woman is different. Some may gain a bulk of the weight upfront, some might be gradual, and some might gain most of it later in pregnancy. Try not to compare your pregnancy weight gain with anyone else or even past pregnancies. It can vary so much.
Relief for an Upset Stomach
Unfortunately, this is one of the many fun symprtoms of pregnancy.
If you experience bloating after eating, it could be due to a number of factors.
If you notice it happens after eating raw veggies, try steaming them to help make them easier to digest (without removing the nutrients you and your baby need).
You can also focus on chewing your food very thoroughly until it’s almost liquid. This makes your food easier to digest and less likely to cause bloating.
Nearing the end of your pregnancy, it’s not uncommon to experience constipation or discomfort with bowel movements. To ease symptoms, try drinking more water, increasing your fiber intake, and supplementing with magnesium.
If you’re still having trouble at this point, you may want to try a laxative and stool softener (after consulting your doctor). A laxative or stool softener can make passing bowel movements easier, which in turn may help reduce the risk of hemorrhoids.
Many physicians, caregivers, and midwives suggest taking supplements to aid in digestion near the end of the third trimester. Be sure to consult with your doctor to ensure safety when selecting brands and determining dosage.
Supplements
During the third trimester, your supplement routine will look almost identical to that of your second trimester. Consider talking to your doctor about making these two little changes:
- If you are constipated, consider supplementing with 500 mg of magnesium per day.
- When you are four weeks out from your due date, drop your intake of fish oil to no more than a half of a teaspoon (or two 1,000 mg capsules) per day.
Wrapping Up
Pregnancy can be very difficult! The fatigue, morning sickness, etc. Give yourself grace and just do the best you can. Don’t stress about being perfect.
I really hope this guide has been useful and that you are feeling strong, healthy, and excited as you move into the final stages of pregnancy and beyond!
Christy
References
- Wolfram, T. Healthy Weight during Pregnancy. Eat Right Academy of Nutrition and Dietetics. February 22, 2017.
- Institute of Medicine. 2005. Dietary Reference Intakes for Water, Potassium, Sodium, Chloride, and Sulfate. Washington, DC: The National Academies Press. https://doi.org/10.17226/10925. https://www.nap.edu/read/10925/chapter/1
- Health Psychol Rev. 2015 Aug 7; 9(3): 323–344.
- Maternal caffeine consumption during pregnancy and the risk of miscarriage: A prospective cohort study. American Journal of Obstetrics and Gynecology, 198, e1-8.. Weng, X., Odouli, R. & Li, D.K. (2008).
- Fetal alcohol syndrome: What you should know about drinking during pregnancy. Paediatrics & Child Health, Volume 7, Issue 3, 1 March 2002, Pages 177–178, https://doi.org/10.1093/pch/7.3.177. https://academic.oup.com/pch/article/7/3/177/2658397
- Arbuckle TE, Liang CL, Morisset AS, Fisher M, Weiler H, Cirtiu CM, et al. Maternal and fetal exposure to cadmium, lead, manganese and mercury: The MIREC study. Chemosphere. 2016 Nov;163:270-282. doi: 10.1016/j.chemosphere.2016.08.023. Epub 2016 Aug 16. http://www.sciencedirect.com/science/article/pii/S0045653516310402
